COVID-19 is a respiratory disease caused by a virus named SARS-CoV-2. COVID-19 means “coronavirus disease identified in 2019.” Sometimes, people use coronavirus and COVID-19 interchangeably, but they are distinct things: One is a virus, and one is a disease caused by the virus.
General information on COVID-19 can be found on our FAQ page.
COVID-19 in the human body
Not all coronaviruses react the same in the human body. This particular virus can lead to COVID-19, which may or may not produce symptoms in people.
The most common symptoms people have are:
- Fever
- Cough
- Loss of smell or taste
- Muscle aches or chills
- Sore throat
- Shortness of breath
If you have these symptoms, you should get tested for COVID-19.
Breathing doesn’t just feel good to you
Here’s what happens in the human body to bring on symptoms like those mentioned above, specifically, shortness of breath. These symptoms can come on rapidly.
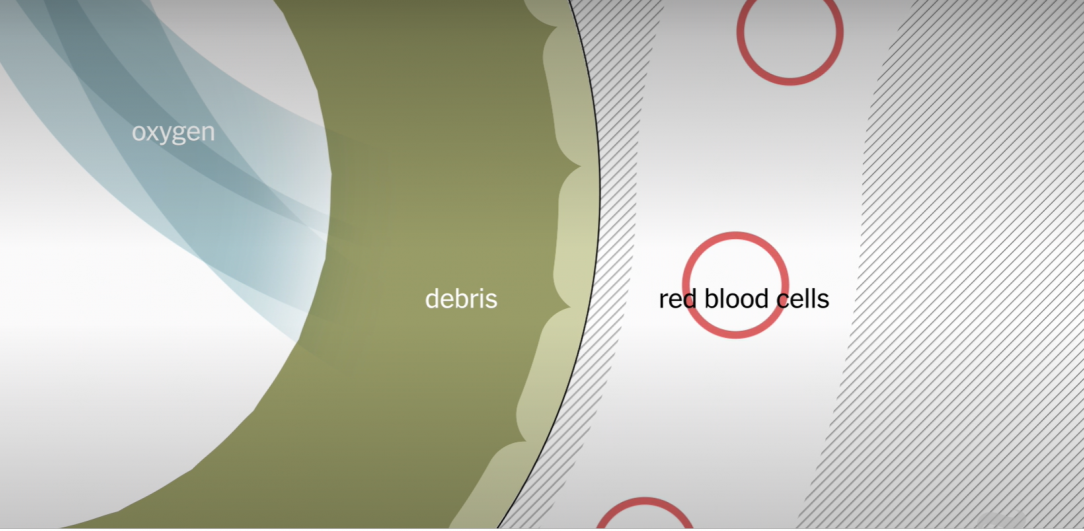
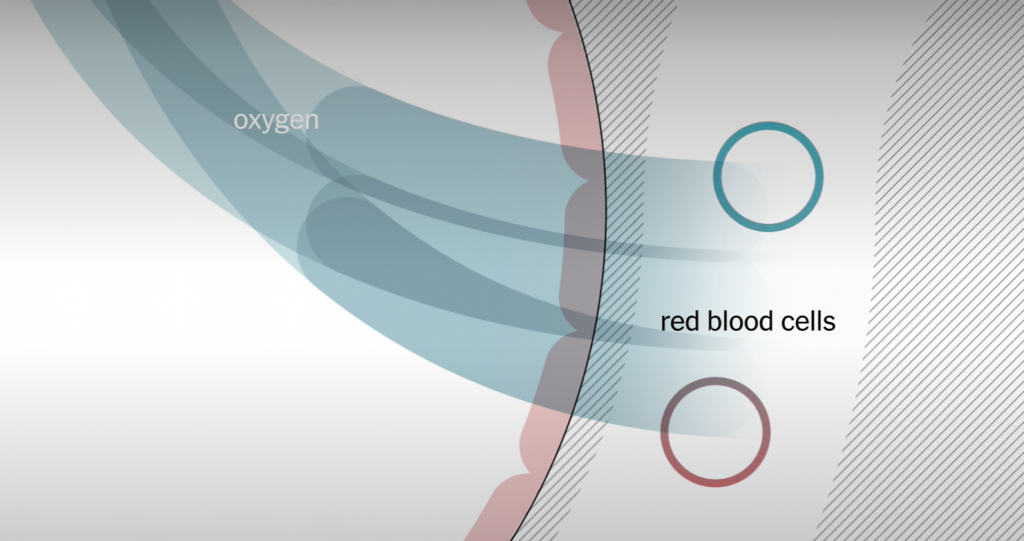
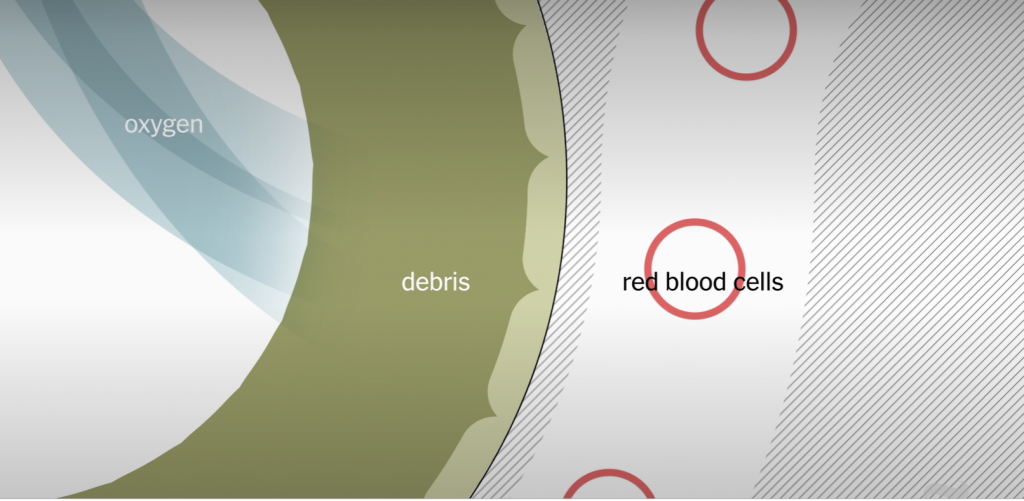
According to the American Lung Association, it is thought the lungs are the first body organ affected by COVID-19. In the early days of a case of COVID-19, the disease can attack important cells in our lungs.
COVID-19 is thought to attack the epithelial cells lining the airways — that catch and clear out things like pollen and viruses — flooding our airways with debris and fluids.
American Lung Association
If a lung infection is severe enough, it can become ARDS – Acute Respiratory Distress Syndrome. ARDS means that the critical and efficient job the lungs normally perform for the body — removing carbon dioxide from your blood and replacing it with oxygen — is depleted.
A Chicago woman who had COVID-19 is recovering after a double lung transplant in June (Via USA Today, includes a photo of her diseased lung)
Normal, healthy breathing doesn’t just feel good to you. It’s doing vital work for your body. ARDS has an effect on the body like drowning without ever going under water. The body begins to strain to breathe to get oxygen to the blood and the skin can begin to turn blue.
In April, the New York Times put the following visualization and interviews together so people could see how COVID-19 attacks the lungs.
Obviously, if this goes on long enough without a resolution, a life-threatening condition known as sepsis can set in and oxygen-starved organs begin to fail, followed by death.
“I had never seen something like this”
The Washington Post reported in July that pathologists (scientists who study the causes and effects of disease) are learning, through autopsies, about other effects of COVID-19, such as microclots in the lungs and other organs. Some of these microclots appear to start early on in an infection.
One pathologist from Louisiana, Richard Vander Heide, who has been performing autopsies since 1994, told the Washington Post, “I had never seen something like this.” His autopsies on people who had died from COVID-19 found a pattern of hundreds or thousands of microclots in the lungs. His discovery has led to medical treatment of blood thinners for COVID-19 patients.
Other effects on organs include brain damage from oxygen deprivation and microclots in the brain.
This doesn’t happen in every COVID-19 case. We know that most people who develop COVID-19 will have mild or no symptoms. Most people (more than 99%) will survive.
But we still don’t know what it truly means to recover from COVID-19. Some people who survive a case of COVID-19 return to normal, healthy lives.
Some still experience a loss of smell and taste for months afterward. Others, who have become known as long-haulers, continue to have medical struggles for many months after an initial infection and continue to experience coughing, tightness in the chest, shortness of breath, diarrhea and fatigue.
The medical science community is still learning more about why this is happening, and we hope to have more certainty one day.
It’s up to each of us
We still need to take medical and health guidance seriously.
If you are sick or test positive for COVID-19, please stay home. We need to continue working to slow the spread of the disease to those who are at risk for a severe reaction to the disease. Those people generally already have one or more health conditions that could become worse if they develop COVID-19.
We recently produced the following two videos to help people understand the difference between quarantine and isolation and when to follow the guidance for each condition.
What is quarantine?
What is isolation?
Also, as we head into the fall, influenza vaccines are becoming available. Please make sure to get an influenza vaccine. Though the influenza vaccine doesn’t prevent COVID-19, we need fewer people to go to the hospital with influenza this year.
We are striving to limit the number of people who go to the hospital with either COVID-19 or influenza. This helps hospitals provide the best care for those who absolutely need it.